Interventional Procedures
Interventional cardiology is a subspecialty that uses catheter-based, minimally invasive techniques to diagnose and treat structural heart disease, coronary artery disease, and certain electrophysiological conditions.
It replaces or complements many traditional open-heart surgical procedures with faster recovery and lower risk.
All interventional Procedures will be performed in one of the affiliated hospitals either by Dr. Sossou or trusted partners

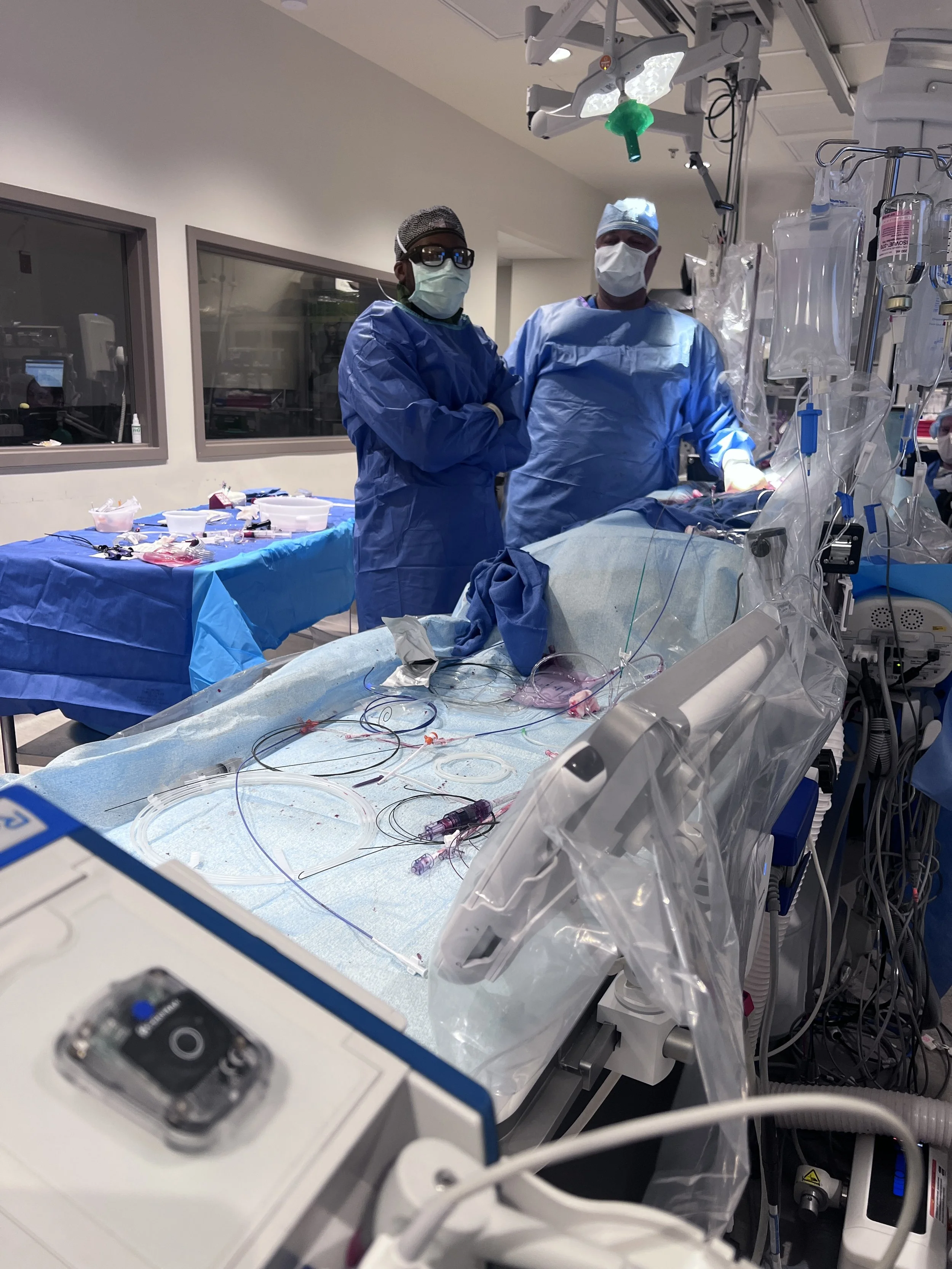
From opening blocked arteries during a heart attack to replacing heart valves without open surgery — interventional cardiology has revolutionized cardiovascular care.
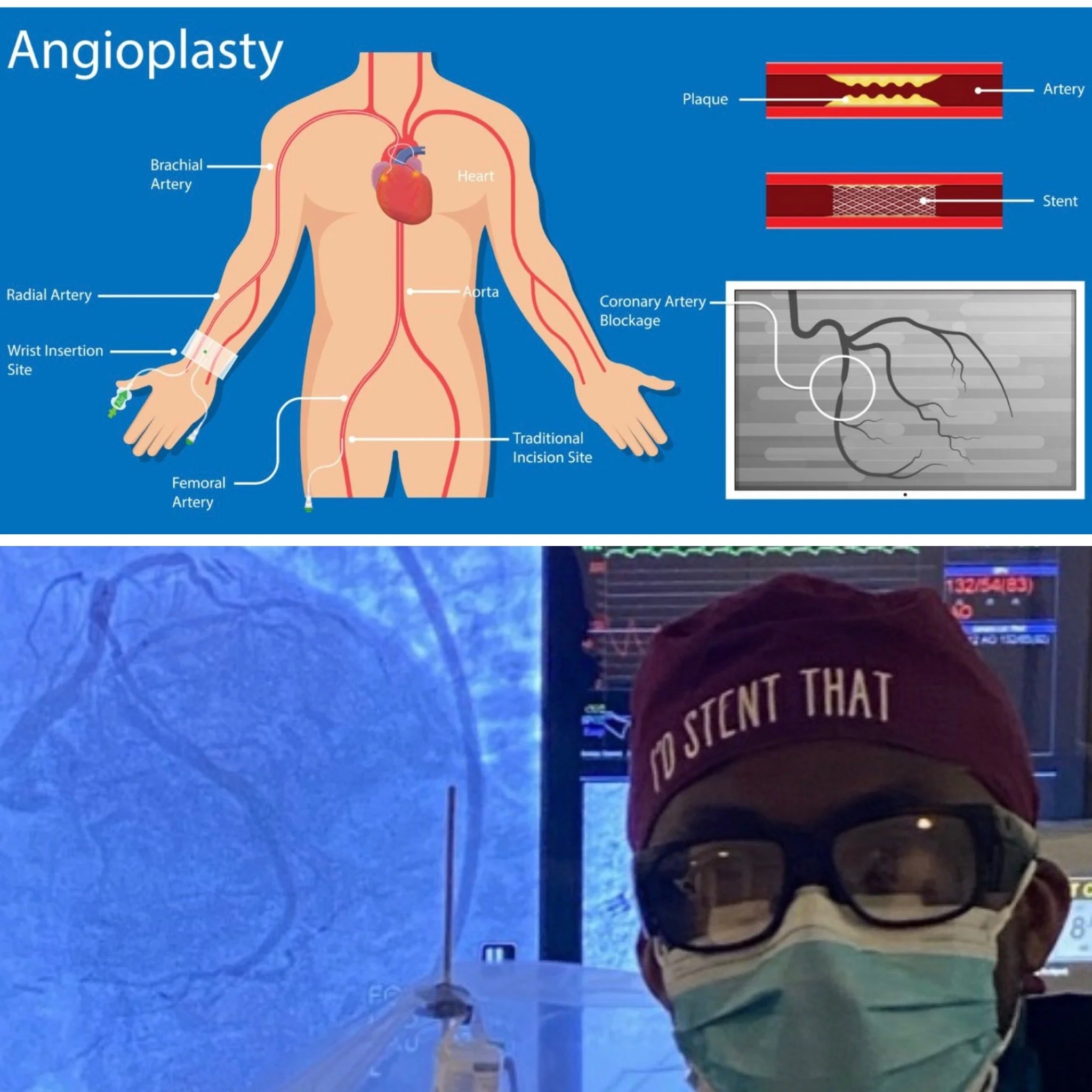
Key Procedures
-
Alcohol injection thins septum in hypertrophic obstructive cardiomyopathy.
Relieves obstruction without surgery.
-
Balloon opens narrowed valves (mitral/aortic/pulmonic). Via groin/arm.
-
Angioplasty and Stenting: Uses a balloon to widen narrowed arteries and places a stent to keep them open, often for peripheral artery disease or coronary blockages
Thrombectomy: Removes blood clots from arteries or veins using catheters, often for stroke or deep vein thrombosis
Carotid Artery Stenting: Places a stent in the carotid artery to prevent strokes caused by narrowing
-
Seals appendage for AFib stroke prevention (no long-term blood thinners). Device via groin vein. ~1 hr; anesthesia; next-day discharge. Off blood thinners after 6 weeks.
-
Edge-to-edge clips for mitral regurgitation.
Placed via groin vein. 1-2 hrs; anesthesia/echo; 1-2 day stay.
Reduces leak, improves symptoms
-
Plugs heart wall hole to prevent strokes. Device via groin vein. ~1 hr; sedated; same/next-day discharge
-
Angioplasty/stenting for heart attack or chest pain due to blockages in the heart arteries.
Balloon inflates, stent placed via wrist/groin.
Restores flow, relieves symptoms.
-
Groin artery valve replacement for aortic stenosis.
New valve deployed inside old one. 1-2 hrs; sedated; 1-3 day stay.
